Yeni knew something was wrong when she woke up feeling nauseous on a September morning at a shelter on the South Side. Her baby was moving, but Yeni barely could.
After sending a few texts to her husband and a volunteer she had recently met, Yeni, a migrant from Venezuela who had entered the United States at the Texas border just two weeks earlier, heard the siren of an ambulance.
She stiffened.
The 33-year-old expectant mother had no car. She knew no number for a clinic or hospital. None of her neighbors, all migrants new to the city, seemed to have any information, either. Nine months into her pregnancy, Yeni had barely seen a doctor. And now her baby, she feared, was ready to come.
Regular prenatal care is a long-established medical protocol that protects the health of mothers and babies. Yet beyond putting expectant mothers on a priority list for shelter, Chicago “does not have specific protocol in place relating to women who arrive pregnant,” said Mary May, a spokesperson for the city of Chicago’s Office of Emergency Management and Communication.
And many migrant women appear to not be getting medical care, according to interviews with new arrivals, volunteers and medical professionals across the city.
The chaos regarding prenatal healthcare underscores Chicago’s struggle to offer basic services to the 15,000 migrants who have arrived since August 2022.
According to the official tallies, the city gives Cook County Health a list every night of 75 to 100 new arrivals to see in the county’s Northwest Side clinic. That includes children who need vaccines, migrants with chronic or acute health issues and pregnant women.
So far, Cook County Health, the designated medical provider for new migrants, says it has seen 241 pregnant women.
But neither the county nor the city can provide estimates of how many pregnant women have migrated to Chicago in the past year nor what percentage of expectant mothers has been seen by medical professionals.

Without much information available, fear and rumor have taken root.
“I talk to other women in the shelter, and we share our experiences,” said Yeni, who delivered her first two children via Cesarean section in her home country. “I’m scared I will go into labor in the shelter without having a date for a C-section. Anything can happen in an operating room. But, if I put my faith in God, I feel it will be OK.”
No guarantee of seeing a doctor
Pregnant migrant women fortunate enough to end up on the county health list are ushered through routine prenatal care — checkups, ultrasounds, blood work.
Who ends up on the list appears to depend on where a pregnant woman lands in the city. Women temporarily living in longer-established shelters — such as Yoxibel, 23, who is staying at the Broadway Armory in Edgewater — report they have been receiving care. Yoxibel, like other mothers in this story, are identified only by their first names because of their precarious immigration status.
By September, she had, with the help of a city social worker, already visited the doctor for three prenatal appointments and gotten the first of four iron infusions to treat her anemia.
Yoxibel also received free rides to every doctor visit. All she had to do was call a number in her phone, and a car would arrive to take her to the Cook County clinic. Yoxibel said the care offered a sense of stability.
“I have nowhere to live, and my back hurts from sleeping on cots,” Yoxibel said in Spanish. “But they told me the baby is doing well. I hope for a boy.”
Not all pregnant migrants have been so lucky.
Noelismar lives in a South Side shelter and has not visited a doctor. The 20-year-old Venezuelan migrant estimates that she’s about seven months pregnant.
“This pregnancy has been the most difficult experience of my life because I’m all alone here,” Noelismar said, speaking through a translator.
In the absence of protocols and facing language barriers, word of mouth has become the prime way some pregnant new arrivals share precious words of advice. Outside of shelters and hotels, there are parking-lot whispers warning new mothers they will be stuck with big bills. Some believe they won’t be able to leave the country until their child turns 21. Others worry their babies will be taken away.
Rumors like these are one reason Noelismar said she doesn’t want to visit a doctor. She shares a room at a shelter with her sister Maria, who also traveled to the United States while pregnant.
Maria was sleeping in Humboldt Park when she went into labor earlier this year. She gave birth in a hospital — she doesn’t know which one — and a nearby resident suggested Maria use her address to receive her baby’s Social Security card. When the card eventually came, Maria said, so did a bill for $30,000.
Half a year later, Maria has not returned to the doctor nor taken her son to see one.
Maria fears her experience has discouraged Noelismar from seeking care.
“She only wants to go to the hospital when it’s time to give birth,” she said.
Little consistency of care
Still, for pregnant migrants, Illinois isn’t a terrible place to end up. It’s one of only a few states that offer Medicaid coverage to women throughout pregnancy and for as long as one year postpartum no matter their immigration status.
The coverage should make it easy for pregnant migrants to see doctors and nurses. But that has proven difficult for many of Chicago’s asylum-seekers.
Recognizing the scramble and disorganization, many people have tried to step in and connect migrant mothers with care. Jaq Aguilar, a first-year medical student at the University of Illinois Chicago, has spent the past several months helping run the Mobile Migrant Health Team.
Aguilar said about 20 pregnant women who have been seen all were reported to the Chicago Department of Public Health, which then fast-tracks their shelter placement. But the system, Aguilar said, is far from perfect.
“There is really very little preexisting network of care and little communication between groups,” the medical student said. “We’re trying our best, but we’re all reinventing the wheel every time we go.”
May said the city coordinates with several mobile clinics to move pregnant migrant women to shelters better outfitted to support mothers and newborn babies.
Still, playing an outsized role are volunteer networks that have formed on Facebook, through WhatsApp text threads and via email chains. The groups function like an ad hoc Spanish-speaking stork service, one that is nimble, messy and determined to find ways to connect women with the care they need.

Volunteers pitch in
Yeni’s pregnancy came as a surprise. Early pregnancy symptoms made the arduous 3,000-mile trek from Venezuela to the United States even harder.
“It was tough,” Yeni said, speaking in Spanish through a translator. “I had nausea all the time.”
She has seen a doctor twice, once after she crossed the border in El Paso and again in Chicago after a volunteer offered to take her to a nearby clinic.
“People here told me to get my baby bag ready,” she said, “but I have nothing.”
The expectant mother also didn’t have much information about where to go. Yeni’s only plan was to text a volunteer who offered to help.
A week later, Yeni found herself in an alarming limbo, with waves of nausea and dizziness. She rejected the ambulance that volunteers called for her. But her symptoms didn’t improve. News that a pregnant woman needed help quickly reached an active WhatsApp thread of volunteers.
“I can leave my meeting and get there in 10 minutes. I speak Spanish,” one volunteer messaged the group.
Fifteen minutes later, Yeni was on her way to the UChicago Family Medicine Birth Center in Hyde Park. Her baby daughter arrived that night by C-section.
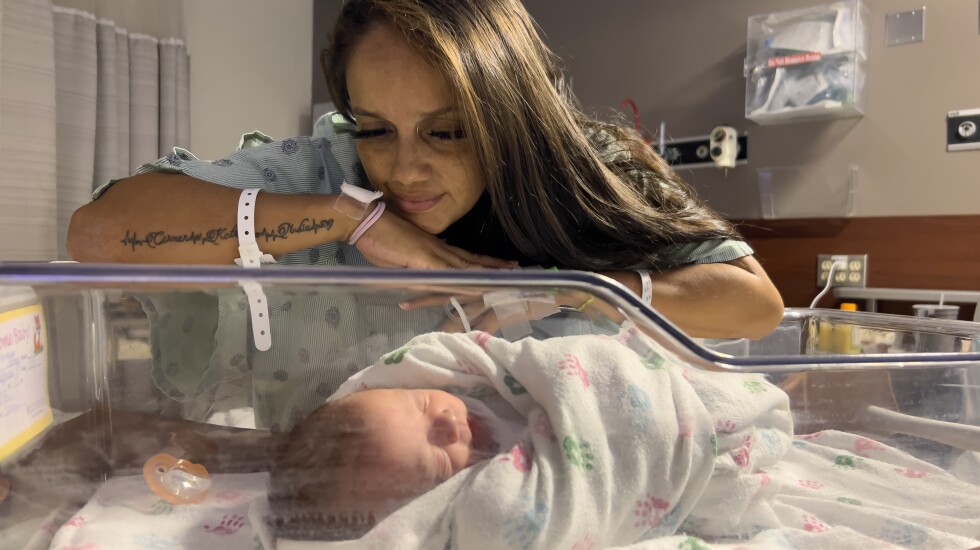
In the following days, Yeni saw a rotating door of nurses and doctors who checked her blood pressure and dosed her pain medicine, and she had meals delivered to her. Her body hurt, and her baby cried often. She longed for her mother, who had been by Yeni’s side during previous births.
Five days after delivery, Yeni and her newborn daughter returned to the shelter where she shares a single room with seven people and sleeps on a bunk bed. Yeni endured a dizzying gauntlet there that’s familiar to any new parent: late-night feedings, dirty diapers and a body that is slow to heal. Outside her window, the long days began to shorten and cool. She turned to her faith and prayed.
Contributing: Cianna Greaves, Molly Morrow
Elly Fishman is the author of WBEZ’s First 12 Weeks series, an intimate look at postpartum recovery for three Chicago-area families, and the book “Refugee High: Coming of Age in America.”








