The patient: A 64-year-old woman in New South Wales, Australia
The symptoms: The woman was admitted to the hospital after experiencing abdominal pain and diarrhea for three weeks. She also had a persistent dry cough and night sweats.
A CT scan of her lungs showed opaque areas where the tissue had thickened, likely due to inflammation or an infection that caused the air spaces in the lungs to fill with fluid, pus or a buildup of white blood cells. The woman also had lesions, or areas of damaged tissue, in her liver and spleen.
When doctors sampled fluid from the patient's lungs, they found an unusually high percentage of eosinophils, a type of infection-fighting white blood cell. At that time, they diagnosed the woman with a rare lung condition called eosinophilic pneumonia and prescribed a daily dose of the steroid prednisolone, which relieved some of her symptoms. They noted that the cause of the lung infection was unknown.
What happened next: Three weeks later, the woman returned to the hospital with a cough and a fever, despite still taking prednisolone, and the lesions on her organs had not healed.
Further tests failed to identify the cause of her respiratory distress. Tissue sample cultures showed no signs of bacterial or fungal infection. Blood work showed that her immune system wasn't producing antibodies to various parasitic flatworms, such as blood flukes (Schistosoma) or liver flukes (Fasciola). Nor was there any evidence of these parasites in her fecal samples.
Doctors advised the patient to continue taking prednisolone and also prescribed her ivermectin, a treatment for parasitic worms, as she had informed the doctors that she'd traveled to countries where such parasites are common.
But her respiratory symptoms did not go away, and they worsened when she attempted to reduce the prednisolone dosage. Her condition continued unchanged for several months.
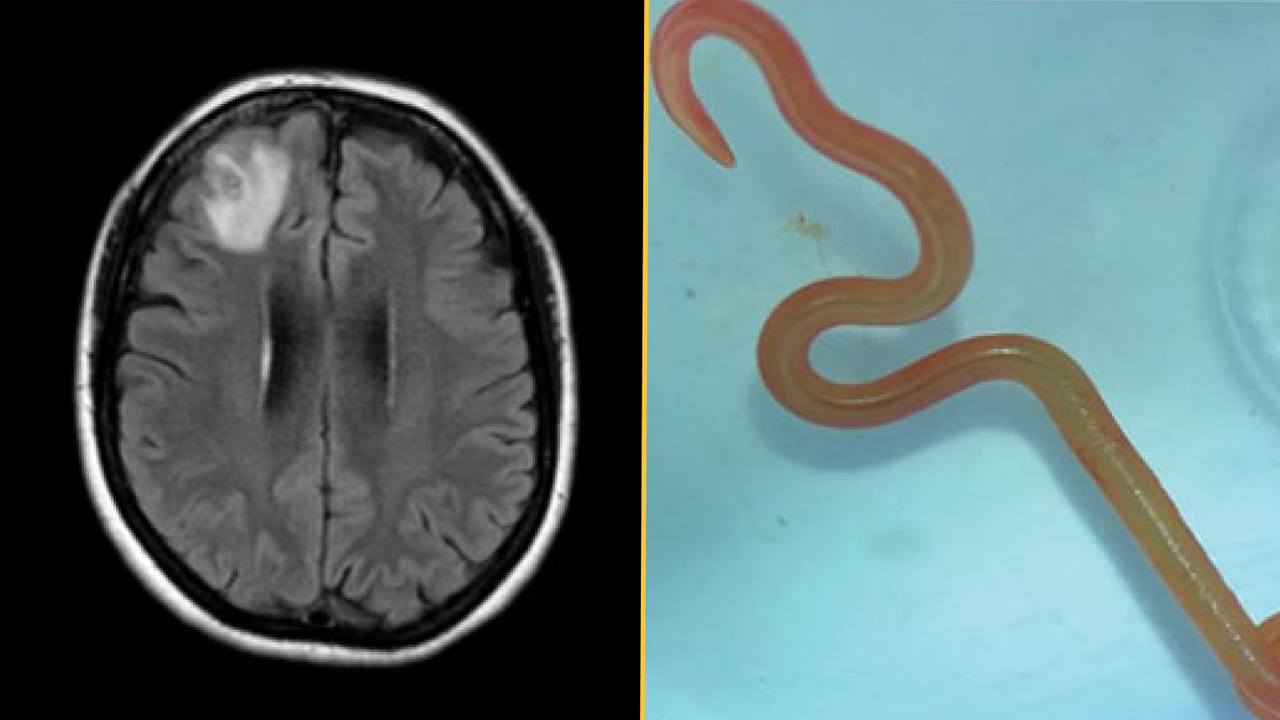
The diagnosis: About a year after her initial hospital visit, the woman began to develop signs of depression and had episodes of forgetfulness. Physicians ordered an MRI of her brain and detected a lesion on the right frontal lobe. They then performed an open biopsy to expose and examine the damaged area. That's when they discovered "a stringlike structure" inside the lesion, which they identified as a living parasitic worm called a helminth, according to a report of her case.
The worm was bright red and measured about 3 inches (80 millimeters) long and 0.04 inches (1 millimeter) thick.
The treatment: Doctors removed the helminth from the woman's frontal lobe and examined the surrounding tissue, where they found no more parasites. They gave her ivermectin for two days, this time in combination with a four-week course of albendazole, a broad-spectrum drug for treating helminth infections, to kill any lingering parasites in her organs.
Albendazole is absorbed by the central nervous system more quickly than ivermectin is, and these drugs have previously been used together to treat nematode infections in humans and snakes. The patient also received a 10-week course of the corticosteroid dexamethasone, to prevent additional inflammation.
Six months after the surgery and three months after the end of the dexamethasone course, the lesions in the patient's lungs and liver were gone, her white blood cell count was normal, and her neuropsychiatric symptoms had improved.
What makes the case unique: The doctors identified the helminth as a third-stage larva of Ophidascaris robertsi, a type of parasitic nematode native to Australia. The adult worms reproduce inside carpet pythons (Morelia spilota), but the nematode can infect other animals during the larval stages of its life cycle.
Carpet pythons were common near the woman's lakeside home, and although she did not recall having any direct contact with snakes, she often foraged wild greens for cooking. She likely became infected after touching or eating plants contaminated by O. robertsi eggs, the case report authors suggested. After the eggs hatched, the larvae migrated to her organs.
The longevity of this larval infection wasn't unusual, as laboratory rats can host O. robertsi larvae for more than four years, according to the report. However, no human infection by this parasite had ever been documented, nor had the parasite's larva ever been found in the brain of its host.
For more intriguing medical cases, check out our Diagnostic Dilemma archives.
This article is for informational purposes only and is not meant to offer medical advice.








